Head and Neck Cancer
Head and Neck Cancer Screening
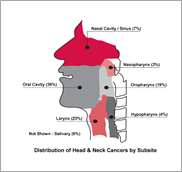
What is Head and Neck Cancer?
Cancers that start in the head and neck are called head and neck cancer. All cancers are named after the area of the body where the cancer starts. Some of the areas of the head and neck where cancer can start are highlighted in the diagram to the right. Cancer happens when cells in the body start to grow out of control. Cancer can happen in nearly all cells of the body and can spread to other parts of the body.
Graphic copied from Head & Neck Cancer Alliance need permission to use.
What are the Risk Factors for Head and Neck Cancer?
- Tobacco – all forms; cigarettes, snuff, pipes, chewing tobacco, snus, cigars, and all vapor products. Tobacco use increases the risk of head and neck cancer by 15 times than people who do not use tobacco.
- Alcohol – heavy use increases the chances of developing cancer.
- Tobacco and Alcohol – use of tobacco and alcohol creates a greater risk of developing cancers than in people who use either alcohol or tobacco alone.
- Human Papillomavirus (HPV) – infection can develop into cancer.
- Oral Sex – with one to five partners over lifetime doubles the risk of HPV infection and cancer. The risk increases five-fold with six or more oral sex partners compared to people who have not had oral sex. Even people who have had sex with only one person in their lifetime can get HPV.
- Gender – men are more likely to get oral cancer.
- Age - oral cancer appears more in people over the age of 40 but has appeared in younger people and children.
- Sun Exposure – cancer in the lip can be caused by sun exposure.
- Diet – low consumption of fruits and vegetables may play a role in oral cancer.
- Oral Health – poor oral health and missing teeth may promote the development of oral cancer.
Why is HPV a Risk for Head and Neck Cancers?
HPV and co-infections are very common. About 80 million Americans are currently infected with HPV and about 14 million people will get a new HPV infection every year according to the Centers for Disease Control and Prevention (CDC). HPV infections clear up most of the time without causing problems. If an HPV infection does not clear up and stays in the body, it may cause cancer later in life.
“More than half of all sexually active people contract one or more types of this virus at one time, making it the most common sexually transmitted disease in the U.S. In fact, oral, head and neck cancers associated with HPV are on pace to overtake the incidence of cervical cancer by the year 2020,” according to the Head and Neck Cancer Alliance (HNCA).
What are the Symptoms of Head and Neck Cancer?
The American Dental Association (ADA), National Cancer Institute (NCI) at the National Institutes of Health (NIH), CDC, American Cancer Society (ACS) plus other agencies/organizations recommend you see your dentist or doctor if the following signs or symptoms in the mouth, throat or lip do not go away after two weeks.
- A sore, lump, irritation, rough spot, crust, or thick patch that does not go away
- Red or white patches on gums, tongue or inside the cheek
- Pain, tenderness or numbness in mouth, tongue, other areas of the mouth or lips
- Difficulty chewing, swallowing or speaking
- Change in voice or hoarseness
- Swelling of the jaw that changes the way teeth fit together
- Unusual bleeding in mouth, nose or throat
- Pain in neck or throat, headaches or ringing in ears
- Blocked sinuses that do not clear or chronic sinus infections that do not clear when treated with antibiotics
- Trouble or swelling with eyes
- Swelling around the jaw and under the chin
Types of Head and Neck Cancer
There are many types of head and neck cancers. Below is a list of the common types.
- Oral cavity cancer – starts in the mouth
- Oropharyngeal cancer – starts in the back of the mouth or throat
- Nasal cavity cancer – starts in the opening behind the nose, a space that runs along the top of the roof of the mouth and then turns downward to join the back of the mouth and throat
- Paranasal sinus cancer – starts in the openings called sinuses that are around or near the nose
- Nasopharyngeal cancer – starts behind the nose in the upper part of the throat
- Laryngeal cancer – starts in the voice box or larynx
- Hypopharyngeal cancer – starts behind the voice box in the lower part of the throat
(List is from If You Have Oral or Oropharyngeal Cancer - American Cancer Society)
How Can My Dentist Help Detect Head and Neck Cancer Early?
- During regular exams, the dentist will ask about changes in your health and if you have had any new or unusual symptoms.
- When your dentist checks your oral cavity, they will examine your lips, gums, tongue, inside of the cheeks, and floor and roof of your mouth. The dentist will also check your throat, tonsils and soft part of the roof of your mouth. The dentist will feel your jaw and neck for lumps or anything not normal. If the dentist does not perform an oral, head and neck exam, ask him or her to do the exam.
Head and Neck Cancer Treatment
What Happens if My Doctor Finds Something Suspicious?
Do not panic! The dentist will not be able to tell if what he or she is seeing is cancer or not. The dentist might ask you to return in a week or two to check you again to see if the area has healed. Your dentist may refer you for testing the day of your checkup or after the second checkup.
Head and Neck Cancer Prevention
What Can I Do to Prevent Head and Neck Cancer?
Get the Vaccine for HPV
- For maximum protection against HPV, vaccinate girls and boys between ages 9 to 12 with 2 doses of the vaccine.
- If you are 26 years or younger consult your dentist or doctor about the vaccines for HPV. People ages 27 to 45 may also receive the HPV vaccines if considered to be at high risk for HPV infections.
Screen Regularly
- Regularly see the dentist and doctor for checkups that include exams for head and neck cancers. Early detection may create better treatment outcomes if cancer is found.
- Perform monthly self-exams. Self-exams of your head and neck help you know what is normal for you. Doing the exam each month helps you find any changes that will need to be examined by a dentist or doctor.
Be Aware of Risk Factors
- Be aware of your risk factors. Men are more likely to get head and neck cancer as they get older.
- If you have a poor diet, eating more fruit and vegetables may decrease chances of developing cancer.
- Stop using tobacco products and reduce or eliminate alcohol consumption to reduce the risk of cancer in the oral cavity and larynx. Studies have shown that people who stop smoking cigarettes lower their risk of head and neck cancers in half (50%) within 5 to 9 years. Twenty years after people have stopped smoking lowers the risk to the same as for people who have never smoked. Studies have also shown that stopping alcohol use will decrease the risk of head and neck cancers.
- Condoms used correctly and a new one used every time during sex can provide some protection. Condoms do not cover every possible HPV-infected area of the body. Condoms should be put on before any contact and kept on until sex is finished.
- Limit the number of sex partners and avoid sex with people who have had may other partners.
Guide to monthly self-exams
- Feel your neck for lumps.
- Using a mirror, look at the inside and outside of your lips and the inside of the cheeks.
- Bite gently and look at your gums.
- Using a flashlight and mirror, open your mouth and look at all sides (top, bottom, sides) of the tongue, back of the throat, the roof of the mouth and under the tongue.
Facts About Head and Neck Cancer
About 3% of all cancers in the United States are head and neck cancers. Men are twice as likely to get head and neck cancers as women are. More of the cancers are in people over age of 40; however, the number of younger people with head and neck cancers is going up. The National Cancer Institute estimates that there could be more than 65,000 cases of head and neck cancers in 2020.
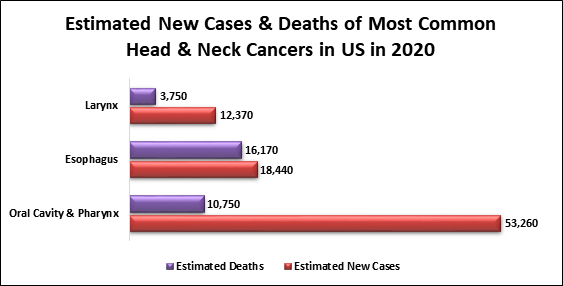
Data Source: American Cancer Society
Oropharyngeal cancer (back of the mouth or throat) caused by HPV infection without other risk factors like tobacco use or drinking has increased dramatically of the last 20 years in young men and women.
Diagnosis of Head and Neck Cancer
Head and neck cancers can be discovered through many different ways. A dentist or doctor may find possible cancers during a routine exam of the head, neck and mouth. Most often cancers are found after a person seeks treatment of a problem or symptoms.
Always share your medical history and any risks you have like tobacco or regular alcohol use. If the dentist or doctor thinks that the problem or symptom needs further evaluation you will be referred to an ear, nose and throat specialist (ENT) called an otolaryngologist or a head and neck surgeon.
The ENT will do a thorough exam. A pharyngoscopy may be used to see some parts of your throat. This can be done in the doctor’s office and is painless. Long-handled mirrors may also be used to see the deeper parts of the throat, the base of your tongue and part of the voice box. A tiny flexible fiber-optic scope may be passed through your nose to see areas of your head that cannot be seen by eyes or mirrors.
If additional tests are need any of the following may be used:
- Panendoscopy – this test will be done under general anesthesia. Scopes will be used to look more thoroughly at the throat, voice box, esophagus (tube to the stomach), trachea (windpipe) and the bronchi (airways off the windpipe in the lungs).
- Biopsy – a small sample of tissue is removed for the problem area. The tissue is examined in a lab to determine if the sample has normal cells or cancer cells and the type of cancer. Several biopsies may be taken.
- Exfoliative cytology – the doctor collects cells from the problem area by scraping it with a small tool. The cells are examined under a microscope.
- Incisional biopsy – a piece of the tissue is cut from the problem area. Depending on the location of the problem area, this may be done in the doctor’s office after the area has been numbed or in the operating room with you asleep.
- Fine needle aspiration (FNA) – the doctor uses a thin, hollow needle and syringe to remove cells from the problem area. The cells will be examined using a microscope. This type of biopsy is used mostly for lumps in the neck or in the lymph nodes.
- HPV Testing – tissues from a biopsy that are squamous cell carcinoma (cancer), especially cells from the tonsil or base of the tongue are tested for the HPV DNA marker called p16. This marker is related to an HPV infection. HPV cancers seem to respond better to treatment than other cancers of the head and neck.
- Blood Tests – blood tests can tell the doctor more about your overall health.
- Imaging Tests – imaging tests may be ordered at different times during diagnosis and treatment to look at the problem area, to see if cancer has spread, to see if treatment is working, and to look to see if cancer has returned after treatment. There are different types of imaging to use and include:
- Chest x-rays – to see if cancer has spread to the lungs.
- CT Scan – provide a detailed view of organs and soft tissue so your doctor can see the location of any tumors, if the tumor is growing into other tissue or if the cancer has spread to lymph nodes, lungs or other organs. CT Scans also provide a detailed look at facial bones to see if they are affected by cancer.
- MRI – images are useful to examine the neck and brain and the surrounding soft tissues of muscle, fat or along nerves.
- PET Scan – PET scans are used when cancer has been diagnosed to see if the cancer has spread to the lymph nodes or other areas of the body especially if the doctor suspect the cancer may have spread but is not sure where. Sugar that contains a low level of radiation is injected into your blood during a PET scan. Cancer cells absorb more of this sugar than normal cells and are easier to see in the images.
Survivorship
Survivorship care plan help cancer patients that have completed treatment understand how to manage problems that can happen after treatment. Guidelines provide help on how to talk to dentists, doctors and other healthcare providers about follow-up care. Guidelines also have information on how to manage treatment effects.
- Head and Neck Cancer Alliance
- American Cancer Society’s Head and Neck Cancer Survivorship Care Guideline
- Cancer.Net
- OncoLink
- Cancer Survivors
What Happens After Treatment
You will see your cancer doctor for years after your treatment ends. It is important that you go to all of the appointments. The exams and test can help find new cancer or returning cancer sooner, helping you get treatments sooner to stop the cancer.
How to Reduce the Risk of Developing a Second New Cancer?
You are at a higher risk to develop a new cancer possibly in your head, neck, esophagus or lungs if you have been treated for head and neck cancers. A second new cancer is higher in people who use tobacco and drink alcohol. Stop tobacco use, stop or limit alcohol drinking, eat a healthy diet with plenty of vegetables and fruit, lose weight and stay physically active.
Educational Tools & Resources
Learn more about stopping tobacco use:
- National Cancer Institute (NCI) or call 800-4-CANCER (800-422-6237)
- Smokefree – provides tools and tips and special pages for Veterans, women, teens, individuals 60+ and for Spanish speakers
- Tips From Former Smokers or call 800-QUIT-NOW (800-784-8669), 855-DÉJELO-YA (855-335-3569), Mandarin and Cantonese 800-838-8917, Korean 800-556-5564, Vietnamese 800-778-8440
- The Real Cost of Tobacco
- American Cancer Society
Find a Provider
- Ask your dentist or doctor about the vaccine for HPV.
- Children who are eligible can receive free vaccines before their 19th birthday through the Vaccines for Children program
- For help in finding low-cost dental services
Questions to Ask a Doctor Regarding Cancer
- What is my main problem?
- Why do you think what I have is cancer?
- Is there a chance I don’t have cancer?
- Would you please write down the kind of cancer you think I might have?
- What do I need to do?
- What will happen next?
- What tests will I need to have?
- Where will the test be done?
- Who can explain the tests to me?
- How and when will I get the results?
- Who will explain the results to me?
- What do I need to do next?
- Why is it important for me to do this?
For more questions, visit If You Have Oral or Oropharyngeal Cancer | American Cancer Society
Data
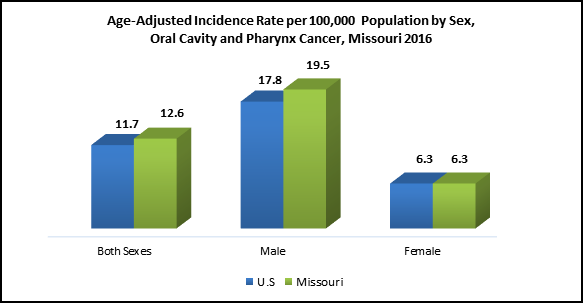
Data Source: United States Cancer Statistics
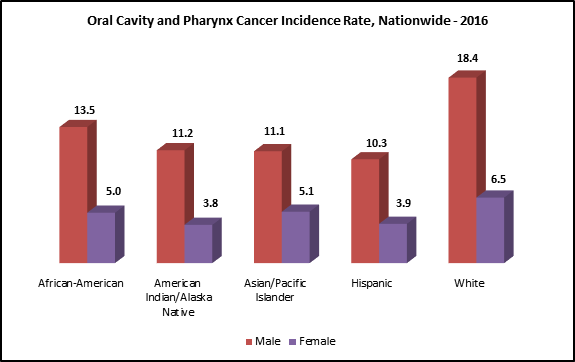
Data Source: United States Cancer Statistics
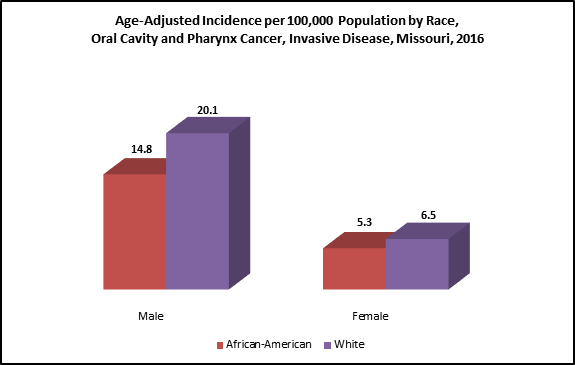
Data Source: United States Cancer Statistics
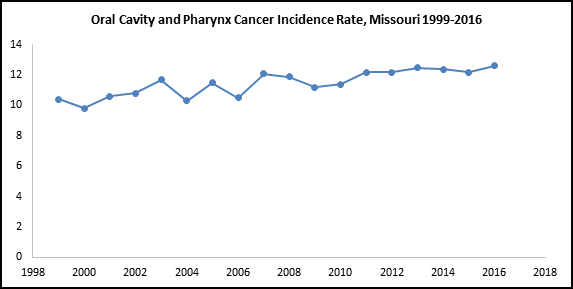
Data Source: United States Cancer Statistics
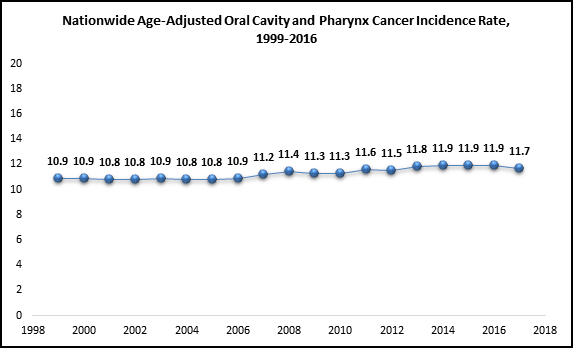
Data Source: United States Cancer Statistics
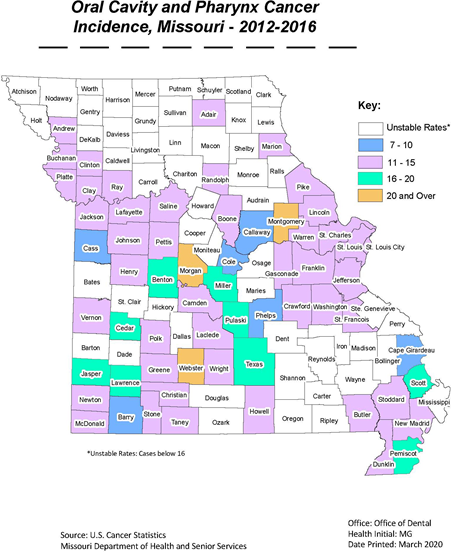
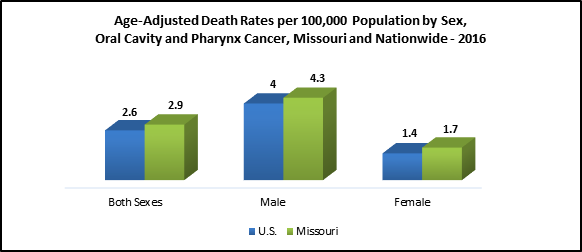
Data Source: United States Cancer Statistics
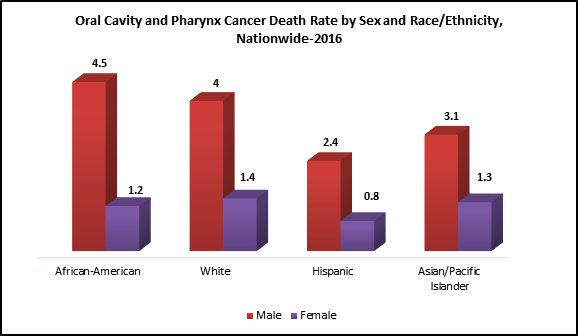
Data Source: United States Cancer Statistics
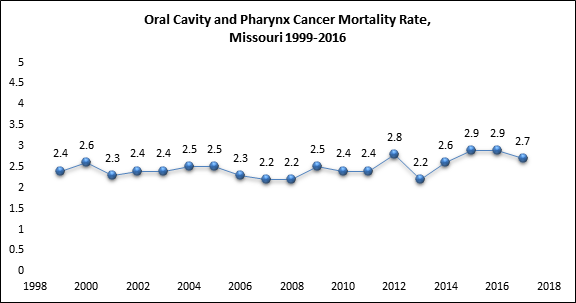
Data Source: United States Cancer Statistics
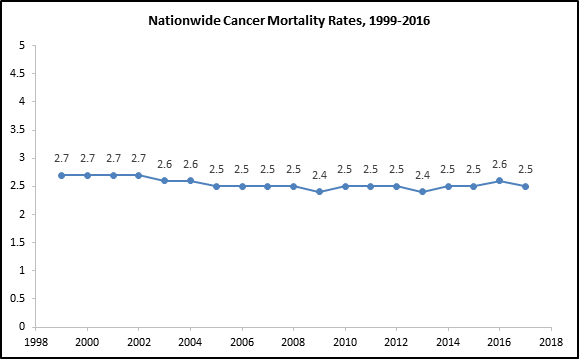
Data Source: United States Cancer Statistics
Sources / Resources
- American Cancer Society (ACS), If You Have Head or Neck Cancer
- ACS, Oral Cavity and Oropharyngeal Cancer
- ACS, Nasal Cavity and Paranasal Sinus Cancer
- ACS, Nasopharyngeal Cancer
- ACS, Laryngeal and Hypopharyngeal Cancer
- American Dental Association (ADA)
- ADA, Oral Cancer
- ADA, Cancer and Dental Health
- ADA, HPV: Head, Neck and Oral Cancer
- ADA, HPV Vaccine and Oral Health
- Centers for Disease Control and Prevention (CDC), Human Papillomavirus (HPV)
- CDC, HPV Diseases and Cancers
- Gut, British Medical Journal, Periodontal Disease, tooth loss, and risk of oesophageal and gastric adenocarcinoma: a prospective study
- Head & Neck Cancer Alliance (HNCA)
- HPV Awareness and Education – HPVANDME, A Non-Profit Organization
- HPV Cancer Resources
- The Oral Cancer Foundation
- National Cancer Institute (NCI) at the National Institutes of Health (NIH)
- NCI, Oral Cavity, Pharyngeal and Laryngeal Cancer Prevention
- NCI, Oral Cavity, Pharyngeal and Laryngeal Cancer Screening
- NCI, HPV Vaccination Linked to Decreased Oral HPV Infections
- NCI, Cigarette Smoking: Health Risks and How to Quit
- NCI, Oropharyngeal Cancer Treatment (Adult)
- NCI, Childhood Oral Cavity Cancer Treatment
- Support for People with Oral and Head and Neck Cancer (SPOHNC) pronounced “Spunk” - Local Chapter in St. Louis that meets in the David C. Pratt Cancer Center at Mercy Hospital St. Louis
- U.S. Public Health Service Chief Dental Officer Newsletter#51: August 18, 2020, Periodontal Disease Linked To Cancer
