Mpox

Mpox is a rare disease caused by the mpox virus. Overall risk to the public remains low. This virus does not spread as easily as others do, such as the virus that causes COVID-19.
Printable Resources
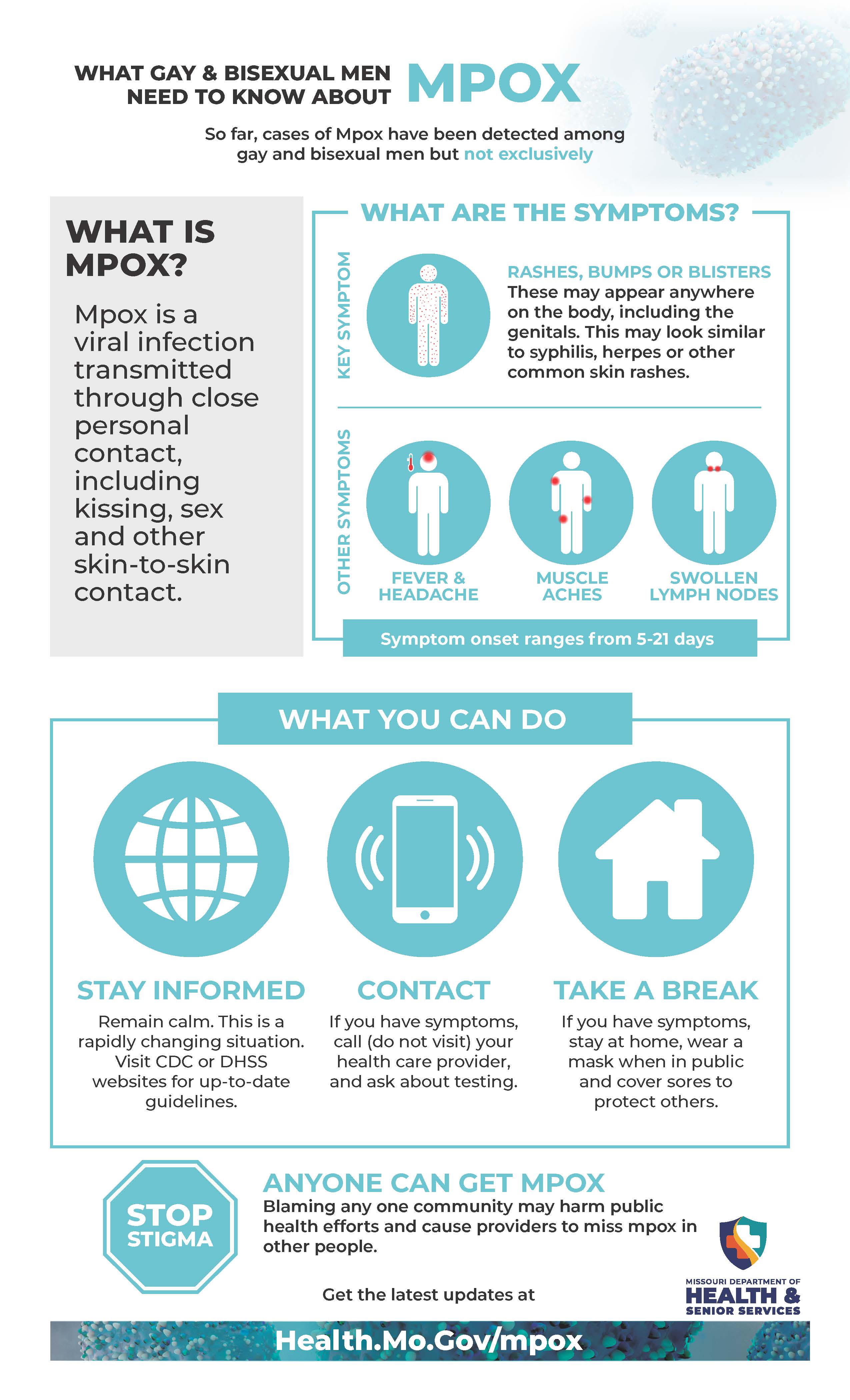
What are the symptoms?
You may experience all or only a few of the symptoms of mpox. Mpox symptoms usually start within 3 weeks of exposure to the virus.
- Most people with mpox will get a rash. Some people have developed a rash before (or without) flu-like symptoms.
- The flu-like symptoms may include fever, headache, muscle aches and backache, sore throat, cough, swollen lymph nodes, chills, or exhaustion.
- If someone has flu-like symptoms, they will usually develop a rash 1-4 days later.
- The rash may be located on or near the genitals or anus but could also be on other areas like the hands, feet, chest, or face.
- The rash will go through several stages, including scabs, before healing. The rash can look like pimples or blisters and may be painful or itchy. The rash may also be inside the body, including the mouth, vagina, or anus.
- The rash will go through several stages, including scabs, before healing. The rash can look like pimples or blisters and may be painful or itchy. The rash may also be inside the body, including the mouth, vagina, or anus.
- The flu-like symptoms may include fever, headache, muscle aches and backache, sore throat, cough, swollen lymph nodes, chills, or exhaustion.
Mpox can be spread from the time symptoms start until the rash has healed, all scabs have fallen off, and a fresh layer of skin has formed. This can take several weeks.
How is mpox transmitted?
The mpox virus is most often spread through direct contact with a rash or sores of someone who has the virus. It can also spread through contact with clothing, bedding and other items used by a person with mpox, or from respiratory droplets that can be passed through prolonged face-to-face contact.
Transmission can happen during sex or other intimate activities, such as:
- Oral, anal, and vaginal sex;
- Hugging, kissing, cuddling and massage;
- Coming in contact with bedding or other items that have the virus on them during or after intimate activity.
How can I get tested?
There is plenty of testing capacity. The Missouri State Public Health Laboratory and many commercial labs have testing capability, and more labs will have testing capability soon. Every healthcare provider should have a plan for getting their patients tested for mpox when they need it.
If you have symptoms of mpox, you should see a health care provider for testing. If you do not have a provider, call local public health agency. You should only get tested for mpox if you are experiencing symptoms.
What should I do if I have a new or unexplained rash (or other symptoms)?
- Avoid sex or being intimate with anyone until you have been checked out by a health care provider. If you don’t have a provider or health insurance, visit a public health clinic near you.
- When you see a health care provider, wear a mask.
What should I do if I (or my partner) have mpox?
- Avoid sex or being intimate with anyone until the rash has healed, scabs have fallen off and you have a fresh layer of skin.
- Cover all sores with clothing or sealed bandages.
- Avoid public gatherings, such as clubs, parties or gatherings until you have talked to a health care provider.
- Wash your hands, sex toys and bedding before and after sex or other intimate activities.
- Stay home and separate from other people in your household.
- If you must leave home for essential needs or medical care, cover your rash and lesions with clothing and wear a face mask.
- Do not share or let others touch your clothing, towels, bedding or utensils. Do not share a bed.
- Do not share dishes, food, drink or utensils. Wash dishes with warm water and soap or in a dishwasher.
- Wash your hands and clean shared surfaces, such as countertops and doorknobs, often.
- Follow the treatment and prevention recommendations of your health care provider.
What can I do to protect myself?
- Avoid close, skin-to-skin contact with people who have a rash that looks like mpox.
- Do not touch the rash or scabs of a person with mpox.
- Do not kiss, hug, cuddle or have sex with someone with mpox.
- Do not share eating utensils or cups with a person with mpox.
- Do not handle or touch the bedding, towels, or clothing of a person with mpox.
- Wash your hands often with soap and water or use an alcohol-based hand sanitizer.
For gay, bisexual and other men who have sex with men, following activities put them at high risk for exposure:
- Having sex or other intimate contact with multiple or anonymous people (such as those met through social media, dating apps, or at parties) increases your risk of exposures;
- Clubs, raves, saunas, sex parties and other places with skin-to-skin or face-to-face contact with many people may also increase risk of exposure, especially if people are wearing less clothing.
Personnel who collect specimens should use personal protective equipment (PPE) in accordance with recommendations for health care settings.
Who should get vaccinated?
Vaccination is an important tool in preventing the spread of mpox. Vaccination reduces the risk of getting mpox and can reduce symptoms if infected. People at risk for mpox should get 2 doses of the JYNNEOS vaccine to maximize protection. The second dose should be administered at least 28 days after the first dose. Those who have already had mpox do not need to get vaccinated. Likewise, routine vaccination for the general public without specific risk factors is not currently recommended.
If an individual is experiencing symptoms of mpox, contact your health care provider for testing or visit the testing resources map. If you have recently been in close contact with someone you think has mpox, you should consult with your health care provider to get the vaccine as soon as possible and no later than 14 days after the exposure.
Mpox Information for Missouri Health Professionals
If a health care provider suspects an mpox case, they should contact their local public health agency, or the DHSS Bureau of Communicable Disease Control and Prevention at 573-751-6113 or 800-392-0272, prior to specimen collection.
Mpox Testing Information – Missouri State Public Health Laboratory
Health Alerts Archive