Definitions
- Abdominal Hysterectomy
- Ambulatory surgery centers (ASC)
- Association for Professionals in Infection Control and Epidemiology (APIC)
- Catheter-associated urinary tract infections (CAUTI)
- CDC
- Central line (CL)
- Central line days (CLDs)
- Central line-associated bloodstream infection (CLABSI)
- Central line-associated bloodstream infection rate
- CMS
- Confer Rights
- Expected number of infections
- Healthcare-Associated infection (HAI)
- Hospital and ASC reporting criteria
- Hospital and ASC reporting period
- MHIRS
- National Healthcare Safety Network (NHSN)
- Public Reporting
- Risk Adjustment
- Significance tests
- Society for Healthcare Epidemiology of America (SHEA)
- Surgical Site Infections
- Standardized Infection Ratio (SIR)
Abdominal Hysterectomy
Surgical removal of the uterus (a hysterectomy) done through an incision made in the abdominal wall. This may also be done by laparoscopy. As opposed to a vaginal hysterectomy, in which the incision is made within the vagina.
Ambulatory surgery centers (ASC)
Are facilities other than hospitals that provide outpatient surgical services. ASCs are required to be licensed by the Department of Health and Senior Services (DHSS) under state law (Section 197.205, RSMo.)
Association for Professionals in Infection Control and Epidemiology (APIC)
A private nonprofit professional organization based in Arlington, VA for healthcare practitioners dedicated to the principles of infection control.
Catheter-associated urinary tract infections (CAUTI)
A catheter-associated urinary tract infection involving any part of the urinary system, including urethra, bladder, ureters, and kidney.
CDC
Federal Centers for Disease Control and Prevention
Central line (CL)
A central venous catheters terminate at or close to the heart, or they may be placed in one of the great vessels such as a large vein in the neck, chest, or groin. CLs are placed by health care professional into a patient and can remain in place for weeks or months. Central lines are used to give patients fluids or medications, withdraw blood, and monitoring the patient's condition. A central line is different from an IV (intravenous catheter) because IVs are placed near the surface of the skin (usually in a small vein located in the patient’s arm or hand). IVs are placed for short amounts of time and thus are less likely to cause a blood stream infection.
Central line-days (CLDs)
The total number of days a central line is in place for each patient in the intensive care unit (ICU). The count is performed each day, and each patient with a central line is counted as a central line-day.
Central line-associated bloodstream infection (CLABSI)
According to the CDC, a CLABSI is a serious infection that occurs when germs (usually bacteria or viruses) enter the bloodstream through the central line.
Central line-associated bloodstream infection (CLABSI) rate
The CLAB infection rate is defined as the number of CLAB infections per 1000 central line-days. If a hospital intensive care unit (ICU) had 5 infections and 100 central line-days, their rate would be calculated as follows:
5/100 = .05 infections per central line-days X 1000 = a rate of 50 central line infections per 1000 central line-days.
CMS
Centers for Medicare and Medicaid Services
Confer Rights
Hospitals and other facilities using the CDC’s NHSN website can share requested data with the Missouri Department of Health and Senior Services (DHSS) using NHSN’s Group function. A facility must first join the “Missouri Group” and then may confer rights to the DHSS. A facility that joins a group does not have access to any data from other facilities in the group.
Expected number of infections
A facility's infection rate is compared to the infection rate of a reference group. This is done by comparing the number of infections reported by the facility to the 'expected number' of infections. 'Expected' in this usage does not mean what we would expect based on something we know about the hospital. Instead, it refers to the number of infections that we would expect if the hospital had the same infection rate as the comparison group.
The expected number is obtained by applying the rate of the comparison group to the number of central line-days reported by the hospital. For example, a hospital reports 4 patients with infections and 500 central line-days. If the rate for the comparison group (all reporting hospitals in the state) is 2.8 CLABs per 1000 central line-days, this equates to a proportion of .0028 (2.8/1000). Applying this proportion to the 500 central line-days results in 1.4 'expected' infections for the hospital (.0028 X 500 = 1.4).
Healthcare-associated infection (HAI)
A healthcare-associated infection is an infection that occurs in a patient as a result of being in a healthcare setting.
Hospital and Ambulatory Surgery Center (ASC) reporting period
The 12-month period during which qualifying facilities must report specified HAI related data to NHSN or the department. For acute care hospitals, these data include CMS specified measures such as the number of central line-days, central line-associated bloodstream (CLAB) infections, Catheter-associated urinary tract infections (CAUTI), and specified surgical site infections (SSIs). During this period, acute care hospitals report CMS required data through the CDC’s NHSN site and ASCs meeting DHSS specified criteria report data directly to the department.
Hospital and ASC reporting criteria
Hospitals are required to meet certain CMS reporting requirements. This requirement includes the reporting of specified HAI data through the CDC’s NHSN website. By April 1 of each year, all ASCs must report the number of selected surgeries performed during the previous calendar year. Facilities are exempt from reporting for any of the selected surgeries where fewer than 20 were performed during the previous calendar year. However, if the facility performs 20 or more of the specified surgeries in the current reporting year, then the data must be reported.
MHIRS
Missouri Healthcare-Associated Infection Reporting System
National Healthcare Safety Network (NHSN)
CDC’s widely used healthcare-associated infection tracking system. NHSN provides CMS, facilities, states, regions, and the nation with data needed to identify problem areas, measure quality of care and progress of prevention efforts.
Public Reporting
The Missouri Department of Health & Senior Services (DHSS) maintains two public reporting websites where users can search data for quality of care indicators related to infections rates for specified surgical procedures. One publicly available website contains over 15 years of historical healthcare associated infection data reported by hospitals and ASCs and another website provides users with a view of more current data. DHSS also publishes an annual statistical report that includes information about HAI data reported by acute care hospitals and ASCs. The statistics found in the annual report are based on data abstracted from DHSS’s MHIRS application, CDC’s NHSN website, and the CMS’s Hospital Compare site. The annual report focuses on CMS IQR data reported by Acute Care Hospitals and ASC data report through MHIRS. Acute care hospitals report data on specified inpatient device-associated and surgical site infections. ASCs report data on specified surgical site infections.
Risk Adjustment
The performance of each facility in preventing Surgical Site Infections has been adjusted to reflect the higher risk of infections associated with certain procedures. Adjusting for these risk levels allows for fairer comparisons among the facilities. If a facility has a high infection rate after the adjustment, viewers of the data can have more confidence that the higher rate is the result of a problem with surgical site infections and not merely the result of treating a large number of high-risk patients.
Here is a detailed look at the basis for the adjustments and how they are calculated:
Risk factor scores for a procedure can vary from 0 to 3, with 3 representing the highest probability of an infection. Risk scores are the sum of scores for three component factors, each of which contributes a 0 or 1 to the total score. The component risk factors that are used in adjusting a facility’s performance are:
- the degree of contamination of the wound at the time of the operation
- the duration of the procedure
- the American Society of Anesthesiologists (ASA) score. This score is an evaluation of the patient’s physical condition.
Occasionally overall risk factor scores are merged, as in “2, 3”. For these surgical procedures, the Centers for Disease Control found that SSI rates were similar whether the overall risk score was a 2 or a 3.
One component, the duration of the procedure, has changed over time. Prior to 2006, the risk score was assigned based on the number of hours needed to complete the procedure. For example, a hip prosthesis procedure that lasted more than 2 hours was assigned a 1, which was then combined with the other two factors to come up with that patient’s total risk score.
Beginning with 2006 and 2007 data, the standard was changed to the 75th percentile of the distribution of durations to determine the point at which a duration factor would contribute a 1 to the overall risk factor score. Under the new standard, a hip prosthesis procedure that lasted more than 123 minutes resulted in a ‘1’ being contributed to the overall risk score. (This data was published in November 2008, Edwards JR, et al, National Health Care Safety Network report, data summary for 2006 through 2007. Am J Infect Control 2008; 36:609-26.)
Missouri does not collect procedure duration data in minutes from the facilities and therefore continues to use the pre-2006 standard based on hours. Data are collected on three procedures for hospitals – hip prosthesis, abdominal hysterectomy and coronary artery bypass with chest and donor incision.
For coronary bypass surgery, the 75th percentile standard published in 2008 is the same as the previous standard – 300 minutes or 5 hours. For hip prosthesis surgery, the national standard is 3 minutes longer than in Missouri -- 123 minutes vs. 2 hours. For abdominal hysterectomy, the standard was 18 minutes longer than in Missouri – 138 minutes vs. 2 hours.
Since Missouri uses the prior standard, this means that Missouri facilities would have slightly higher risk scores for abdominal hysterectomy and hip prosthesis procedures than they would if the 75th percentile standard had been used. For example, a hip prosthesis procedure lasting 122 minutes would result in a ‘1’ being added to the risk score for Missouri facilities because the procedure lasted more than two hours. Facilities using the 123-minute standard would have a ‘0’ added, and would therefore have a lower overall risk score for the same procedure. At some point in the future, we plan to follow NHSN’s lead by collecting procedure duration data in minutes.
To put Missouri’s data into perspective, users often want to make comparisons to U.S. data. For that reason, a column is included in our HAI tables labeled “Hospital Performance Compared with Facilities in U.S.” This column is based on the annual National Health Care Safety Network publications, known as NHSN.
However, hospitals that report to NHSN are not a random sample of hospitals in the U.S., and NHSN’s annual publications do not cover the same time periods as Missouri data, which are updated quarterly. And, as described above, Missouri and NHSN no longer define duration risk the same way. These differences make NHSN data a less-than-optimal basis for comparison. Nevertheless, the department’s staff believes that including a comparison with their data in our tables still helps users put Missouri data into a reasonable context and perspective.
Significance tests
Test for chance factors
Tests of statistical significance are needed to tell us whether the number of infections in an ICU or a facility is unusually high or low relative to the number we would expect if the facility had the same infection rate as a reference group. For example, suppose a relevant reference group (such as all reporting medical ICUs in the state) has a rate of 10 infections for every 1000 central line-days. Then, all other things being equal, a medical ICU that has twice the number of central line-days, or 2000, would be expected to have about twice the number of infections, or 20. However, the ICU is not likely to have exactly 20 infections during the year, and if it has a few more or less, we would attribute it to chance factors and normal fluctuation. If an ICU has many more (or less) than the expected number, we should be less certain that this was due to chance factors. In fact, we should be concerned that this rate is too high and maybe the facility is having a problem with infections. The function of the statistical test, then, is to help us determine at what point we should become concerned--at what point is the high (or low) rate not likely to be due to chance factors.
Significant results
When a statistical test is performed on the number of infections in a facility or ICU and the test suggests that there are fewer infections than expected, or more infections than expected, based on the reference group rate, the results of the test are said to be ‘significant’ or ‘statistically significant’. If the test is performed and the number of infections is found to be within the range of what is expected, the results are said to be ‘statistically insignificant’ or ‘non significant’. Because of the way in which statistical tests are performed, significant results are generally more informative than non-significant results. If a facility does not treat unusually severe patients and it also has significantly more infections than the expected number, it is safest to assume that the facility is having a problem with infections. At least consumers should be concerned enough to investigate further if they are considering treatment at the facility. If a facility treats patients with varying degrees of severity and also has significantly fewer infections than the expected number, then it is probably doing a good job of keeping health care-related infections under control.
Non-significant results
When the number of infections in a facility or ICU is not significantly different from the expected number, the interpretation is more ambiguous. If an ICU has a small number of central line-days or a facility has a small number of surgeries, chance will play a bigger role in the observed infection rate, the number of infections will fluctuate more from year to year, and it is likely that the number of infections will not be significantly different from the expected number. However, the facility could still be doing a poor job or a very good job of controlling infections. If a number of years of data were combined in order to minimize the role of chance factors, the number of infections might be seen to be lower or higher than expected based on the reference group rate for the same number of years.
Confidence Intervals
For the data on this site, the significance tests were done by comparing the expected number of infections to confidence intervals (CI) around the reported number of infections. To oversimplify, the CI expresses the influence of chance on the reported rate. For example, if an ICU had 10 infections for the year, the confidence interval would be 4.7-18.3. If the expected number of infections is lower than 4.7, the CI indicates that 10 is significantly higher than expected; if the expected number is above 18.3, then the CI indicates that 10 is significantly lower than expected; if the expected number is 4.7, or 18.3, or anywhere in between, then the CI indicates that 10 is not significantly different from the expected number.
The confidence intervals are exact poisson confidence intervals calculated by using the inverse gamma function as proposed by Leslie Daly ( 0 infections have a 95% confidence interval of 0 – 3.689.): Daly, L. The Calculation of Exact Binomial and Poisson Confidence Limits; Comput. Biol. Med., Vol. 22, No. 5, pp 351-361, 1992.
Infection Rate Comparisons
Tests of significance are needed to tell us whether the number of infections in a facility is unusually high or low relative to the number we would expect if the facility had the same rate as a reference group. One type of significance test consists of calculating a confidence interval (CI), or range of values, around the number of infections in the facility. This CI can be thought of as the typical fluctuation in the number of infections in the facility. For example, the number of infections might be 10, with a CI of 5-15. This CI is then compared to the expected number of infections that we have calculated. If the expected number falls within the CI (between 5 and 15), the facility rate and the reference group rate are considered to be similar. In such cases, the ASC will have a circle that is half full ( ) in the ASC Comparison tables. If the expected number is above the CI (any number above 15 in this example), the facility rate is considered to be significantly lower than the comparison group rate, and the ASC has a full circle (
) in the ASC Comparison tables. If the expected number is above the CI (any number above 15 in this example), the facility rate is considered to be significantly lower than the comparison group rate, and the ASC has a full circle ( ) in the tables. If the expected number is lower than the CI (any number below 5 in this example), then the facility rate is considered to be higher than the comparison group rate, and the ASC has an empty circle (
) in the tables. If the expected number is lower than the CI (any number below 5 in this example), then the facility rate is considered to be higher than the comparison group rate, and the ASC has an empty circle (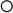 ).
).
Society for Healthcare Epidemiology of America (SHEA)
A professional society that improves public health by establishing infection prevention measures and supporting antibiotic stewardship among healthcare providers.
Surgical Site Infections
Surgical Site Infections (SSIs) are infections that are directly related to an operative procedure. Some SSIs are minor and only involve the skin or subcutaneous tissue. Other SSIs may be deeper and more serious.
Standardized Infection Ratio (SIR)
A summary measure used to track HAIs over time at a national, state, or facility level. It adjusts for various facility and/or patient-level factors that contribute to HAI risk within each facility.
